Development of Patient-Specific Adaptive Assistive Devices for Brachial Plexus Injury
Corresponding email: halim471@uitm.edu.my
Published at : 05 Feb 2024
Volume : IJtech
Vol 15, No 2 (2024)
DOI : https://doi.org/10.14716/ijtech.v15i2.6708
Rashid, H., Haremy, C.M., Othman, A.D., Hashim, N.M., Izmin, N.A.N., Abdullah, A.H., 2024. Development of Patient-Specific Adaptive Assistive Devices for Brachial Plexus Injury. International Journal of Technology. Volume 15(2), pp. 404-413
| Helmi Rashid | School of Mechanical Engineering, College of Engineering, Universiti Teknologi MARA (UiTM), 40450 Shah Alam, Selangor, Malaysia |
| Chyesia Moses Haremy | Biomechanical & Clinical Engineering (BioMeC) Research Group, School of Mechanical Engineering, College of Engineering, Universiti Teknologi MARA (UiTM), 40450 Shah Alam, Selangor, Malaysia |
| Ahmad Dzuharuddin Othman | School of Mechanical Engineering, College of Engineering, Universiti Teknologi MARA (UiTM), 40450 Shah Alam, Selangor, Malaysia |
| Natiara Mohamad Hashim | Faculty of Medicine, Universiti Teknologi MARA (UiTM), Sungai Buloh Campus, 47000 Sungai Buloh, Selangor, Malaysia |
| Nor Aiman Nor Izmin | Interdisciplinary Graduate School of Engineering Sciences, Kyushu University, 6-1 Kasuga-koen Kasuga-Shi, Fukuoka, 816-8580 Japan |
| Abdul Halim Abdullah | Biomechanical & Clinical Engineering (BioMeC) Research Group, School of Mechanical Engineering, College of Engineering, Universiti Teknologi MARA (UiTM), 40450 Shah Alam, Selangor, Malaysia |
Injury to the brachial plexus prevents the arm, wrist, and
hand from communicating with the spinal cord in whole or in part. The
'patient's upper arm limb appears to be completely incapable of performing any
type of independent movement. The aim of this project is to design and develop
a customized adaptive assistive device for patients with brachial plexus injury
and to fabricate the prototype using 3D printing technology. The development of
the device involved adapting the mechanical engineering design process,
including conceptual design and finite element analysis, to predict the
performance of the design and to select the best printing materials. The
patient's left arm was 3D scanned to create a customized part that perfectly
fit the patient. The 3D model of the prototype was developed using Autodesk
Fusion 360 and Autodesk TinkerCAD. Two different materials, namely Polylactic
Acid (PLA) and Acrylonitrile Butadiene Styrene (ABS), were considered in the
computational analysis. Results show that the maximum von Misses stress of PLA
is observed at 2.464 MPa, slightly higher than the ABS material (2.451 MPa),
indicating a greater stress tolerance imposed on the material's strength.
However, PLA has a smaller maximum displacement than ABS, at 0.019 mm and 0.030
mm, respectively. The PLA material was chosen for 3D printing based on several
considerations, including mechanical qualities, cost, printing time,
durability, and data evaluation. The adaptive device for brachial plexus injury
was successfully delivered to the patient and demonstrated the capability to
assist in arm movement.
Adaptive assistive device; Brachial plexus injury; Finite element analysis; Patient-specific; 3D printing
An injury to the brachial plexus, the network of nerves that carries impulses from the spinal cord to the shoulder, arm, and hand, is referred to as a brachial plexus injury (BPI), sometimes known as a brachial plexus lesion (National Institute of Neurological Disorders and Stroke, 2008). Injury to the brachial plexus prevents the arm, wrist, and hand from communicating with the spinal cord in whole or in part. Frequently, brachial plexus injuries also leave the area completely numb (Johns Hopkins Medicine, n.d.). Brachial plexus injuries are a major indication of shoulder arthrodesis (Sousa et al., 2013). An injury that suddenly affects these nerves, commonly referred to as a brachial plexus injury, can cause various symptoms such as pain, weakness, numbness, or limited movement in the shoulder, arm, and/or hand (Cleveland Clinic, n.d.).
An assistive device is a device that allows a patient or
user with a disability to perform any daily activity with little to no
assistance from others (Mazlan et al., 2021; Oliver, 2019).
Most patients with illnesses or impairments who receive rehabilitation use
assistive devices. These devices not only reduce
their reliance on caregivers but also enhance their level of functioning and
participation in the community (Levesque and Doumit, 2020). To ensure
the safety of users while using assistive devices, it is crucial to design them
with their limitations in mind. Muscles, which constitute 45% of body weight,
are the predominant type of tissue in the body (Volpi et al., 2022).
With the aid of the nervous system, the muscular system provides the capacity
for movement and performing everyday activities. Due to a lack of product
development experience, medical personnel are having problems creating suitable
assistive equipment that could benefit them. Even engineers who are skilled in
product development lack the medical knowledge necessary to diagnose any issue
that could endanger the patient further (Abas et al., 2023;
Devin et al., 2023; Cutti et al., 2023). The study,
analysis, design, and production of an adaptive assistive device for a patient
with a brachial plexus injury are the focus of this project.
This adaptive aid was created for Patient A, a programmer
with a left arm brachial plexus injury. Due to his left arm's brachial injury,
he finds it challenging to carry out his duties, such as utilising a laptop or
computer while resting his hand on a table. The patient has a history of
brachial plexus damage stretching a few years ago. He is unable to
spontaneously raise his left arm like other individuals. The primary goal of
this study is to develop an orthosis that will allow the patient to raise his left
arm independently without assistance from the other hand. The left limb of the
patient will be 3D scanned to determine how the limb should be shaped for the
device.
The design will be
carried out using commercial computer-aided design (CAD) software, using the 3D
scanned limb as a reference for dimensions (AutoDesk Fusion 360). Before
modelling it in a CAD programme, a few design concepts will be created by
referring to the various adaptive assistive devices that are available to
create the best design under the direction of an expert in rehabilitation. The
study will only concentrate on the Fused Deposition Modelling method of 3D
printing (FDM). In order to achieve the maximum accuracy for the mechanical
properties, the 3D Printing settings will be as follows: 0.1mm layer height,
20% infill, 3 shell layers, and 4 top/bottom layers. For the analysis, only the
commercial program AutoDesk Fusion 360 will be used to simulate Finite Element
Analysis (FEA). Different kinds of materials will not be tested experimentally.
Other options include using 3D Printing technology, which is significantly more
affordable, produces devices more quickly, and allows for patient-specific customisation
(Jonnala,
Sankineni, and Kumar, 2023).
The project starts
with the problem identification from the patient consultation. The concepts can
be filtered by using the Pugh method. The final selection of engineering design
was modelled using CAD software. A static finite element analysis was performed
to predict the product performance before 3D printing fabrication.
2.1. Patient Consultation
In this stage, meeting with the patient was essential to identify and understand the problems before proceeding to generate ideas and concepts to develop a suitable device. The literature review and benchmarking were extensively explored to better understand. Thus, various ideas and concepts were successfully interpreted and generated based on different types of assistive devices (Ahmed and Al-Shammari, 2023; Scherb et al., 2023; Rashid et al., 2012). Figure 1 shows the process flow in this project. The project was initiated by patient consultation with the rehabilitation specialist to identify the problems. The process is followed by a 3D scanning process to capture digitization data of the patient for patient-specific device development. The idea and several concepts were then generated before coming out with a preliminary design. The detailed design was created and analysed computationally before proceeding to the fabrication and testing of the product. In the analysis stage, stress concentration and safety factors were part of the criteria to be considered for the pass-and-fail statement.
Figure 1 Project flow in developing the patient-specific adaptive assistive device
2.2. Conceptual Design
Several ideas to solve the
problem were sketched to get better pictures of the solution. Figure 2 illustrates the
proposed solution, which consists of (a) a harness and (b) an upper and lower
arm holder. The purpose of the holder is to fit the patient's arm securely,
preventing any movement or loosening.
Additionally,
a harness utilizing a customized
strap has been proposed to support the fixation to the patient's body.
2.3. CAD Design and Modeling
3D scanning technology was
adapted to capture the shape of the 'patient's arm. The scanning process was
conducted at the Hospital Al-Sultan Abdullah, UiTM, under observation by a rehabilitation specialist
using a handheld 3D scanner machine (Shining 3D, China). Figure 3(a) shows the
3D scanning process on the left arm (affected arm) of the patient, while Figure
3(b) indicates the raw images of the scanned data. The arm model was
reconstructed and smoothened using Meshmixer software to obtain a precise and
identical shape of the patient's left arm. To ensure that the design seems proportionate, the arm holder
must resemble the geometry of the left arm. CAD software is used to
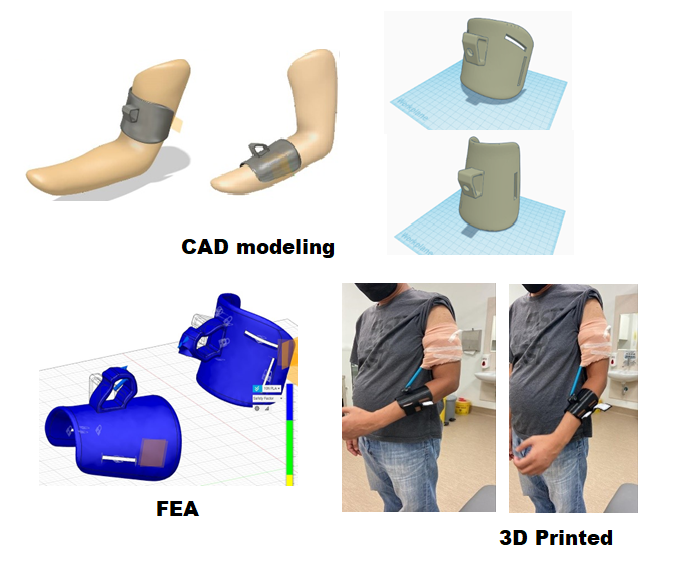
design all parts of the device. Figure 4 illustrates the final design of the
arm orthosis, which consists of two parts: (a) the upper arm holder and (b) the
lower arm holder. After designing the arm using Autodesk Fusion 360, the file
is converted to .stl files and then imported to the AutoDesk TinkerCAD
software, as shown in Figure 5. This is for designing the slot for the
resistance band and straps for the harness to be tied together.
Figure 2 Sketches of the proposed assistive device, which consists of the (a) harness and (b) upper and lower holder
Figure 3 (a) 3D scanning process on the left arm of the patient with the
observation by the rehabilitation specialist, and (b) raw images of 3D scanned
data
2.4. Finite Element Analysis
Computational analysis is the fundamental approach to predicting a 'product's strength, material selection, and optimized design, which is widely used in medical science and engineering design (Hamza et al., 2023; Faadhila et al., 2022; Ahmad et al., 2020, Nor-Izmin et al., 2020; Abdullah et al., 2012). A static finite element analysis was performed to predict the 'product's performance before proceeding to 3D printing fabrication. This provided optimum parameter setting and design. The Autodesk Fusion 360 software was used for the static stress analysis on both upper and lower arm holders to observe the force-loading effects in the resistance band slot area of the holder. Two different materials, namely Polylactic Acid (PLA) and Acrylonitrile Butadiene Styrene (ABS), were evaluated to predict the suitability of these materials for the device.
Figure 4 Designing the (a) upper arm holder and (b) lower arm holder using AutoDesk Fusion 360
Figure 5 Designing the slot for the resistance band and strap
harness for (a) the upper arm and (b) the lower arm holder using AutoDesk
TinkerCAD
Figure 6 illustrates the loading
and boundary conditions conducted in this study. The boundary condition
(constraints) was set on the four-hole slots on the corners for the upper arm
holder and two-hole slots on the corners (labeled in red line) for the lower
arm holder where the strap of the harness is tied. Constraints are applied to a
model to prevent it from moving in response to applied loads. A 10N structural
load/force (labeled blue arrow) was applied onto the slot of the resistance
band where the weight of the upper arm and lower arm react toward each other.
The blue labels indicate the loading condition, while the red labels show the
constraints. The resulting von Mises stress, displacement, and safety factors
were the main focus of this simulation to assess the design's validity in
real-world conditions (Farah, Anderson, and Langer, 2016).
Figure 6
Loading and boundary conditions setting in the analysis
2.5. Fabrication of the Assistive Device
In
the fabrication procedure, both the upper and lower arm holders were created
using a 3D printer capable of working with PLA and ABS materials. The selection
of these materials was based on their widespread availability and common use in
the development of adaptive devices and prototypes, as highlighted in previous
studies (Wahid
et al., 2022; Mazlan et al., 2021). The design
model was generated using Autodesk Fusion360 CAD software and then exported in
stereolithography (.stl) format to the slicing software Ultimaker Cura.
Subsequently, the file was converted into a g-code file for the Creality
Ender-3 V2 after the slicing process. For both arm orthosis components, a
thickness of 5mm and an infill density of 20% were selected for 3D printing
manufacturing. These parameter settings were informed by prior research (Wahid et al.,
2022; Mazlan et al., 2021; Hamzah et al., 2019) while
considering printing cost and orthosis weight. Safety factors and the
weight-to-performance ratio were crucial in achieving a promising product. It's
worth noting that increasing infill values will raise the young modulus and
product weight (Mazlan et al., 2023).
Additionally, PLA filament, chosen for its ease of printing and higher
stiffness compared to ABS, exhibits a tensile strength greater than 37 MPa. The
upper arm holder required 12 hours for printing, while the lower arm holder
took 14 hours.
3.1. Comparison
between PLA and ABS Materials
The performance
of both materials was compared on the resulting von Mises stress, displacement,
and safety factor, as shown in Table 1 (a), (b), and (c), respectively. The
maximum von Misses stress of PLA is observed to be higher in comparison to the
ABS material, indicating a greater tolerance of stress imposed on the
material's strength. However, PLA has a smaller maximum displacement than ABS,
at 0.019 mm and 0.030 mm, respectively. The reaction forces and reaction
moments are often produced by applied force actions. Structure failure can
occur when reaction forces exceed action forces, resulting in fracture and
corrosion. When comparing the two materials in Table 1(a), PLA had lower
maximum reaction forces than ABS, indicating that PLA opposes less force from
the applied force from the detachable arm orthosis, which is also influenced by
gravity force. The most common approach to express a safety factor is as a ratio
between a measurement of the maximum load that will not cause the stated type
of failure and a comparable measurement of the maximum load that is expected to
be applied. The factor of safety is the most straightforward and extensively
utilized strategy in handling variability and uncertainty in engineering design
(Nigro
and Arch, 2023; Moreland, 2009). The application of safety
considerations to ensure that a building can fulfill its intended function
reduces the chance of failure to an acceptable level (Amitrano et al., 2023; Sarma
et al., 2020). Both materials have the same safety factor
of 15, which is relatively high and considerably above one, indicating that
neither material will fail under the current conditions. As a result, PLA is
superior to ABS as a suitable material for producing this arm orthosis. One of
the reasons for choosing PLA is to save cost, and the failure difference
between PLA and ABS does not affect the design of arm orthosis and the
'patient's comfort when using the arm orthosis.
3.2.
Prototype of the Assistive Device
The
prototype of the patient-specific assistive device was successfully developed
and printed. Although the finite element analysis had been conducted earlier,
issues of fit- to-patient and comfort are subjective and need to be tested on
the patient. Therefore, the prototype of the device was essential to observe
the highlighted issues. Design changes, revisions, and improvements were made
to each 3D-printed prototype. The patient's feedback and observations are
critical for obtaining the greatest quality 3D-printed arm orthosis. Table 2
illustrates the changes implemented as a result of patient feedback and
observations during multiple attempts. Furthermore, Figure 7 depicts the
fitting process with the patient, which directly contributes to the enhancement
and modification of the device.
Table 1 Variation of (a) von Mises Stress, (b) Displacement, and (c) Safety factor for the assistive device at different material properties, namely PLA (left) and ABS (right)
Table 2 Changes and modifications of the design model based on the patient feedback
Figure 7
Patient fitting and testing the functionality of the device
A
patient-specific adaptive assistive device for brachial plexus injury has been
successfully developed. Computational analysis was employed to assess the
strength of the arm orthosis under various parameter settings before proceeding
with 3D printing fabrication. This device works in tandem with resistance bands
secured to the arm holders. The final concept design was chosen through a
rigorous conceptual evaluation method. The overall analysis, using different
materials of the same thickness under the same load, indicated that PLA
exhibited the highest stress and the lowest maximum displacement. Subsequently,
the device was fabricated using 3D printing technology, with the choice of
material based on the prior analysis. The resistance band acted as an elastic
force, enabling the patient to perform daily activities more easily. One
notable limitation is that the developed prototype has not undergone
quantitative testing on the patient in this manuscript. At this stage, the
project's focus has been on creating a prototype that offers an ideal fit for
the patient and is functional. Further research is recommended to assess the
performance of the printed product, ensuring the project's continuity and
refinement.
This study was funded by the Universiti Teknologi
MARA through the research grant No. 100-RMC 5/3/SRP (037/2021). We would like
to express our appreciation and gratitude to the College of Engineering, UiTM
and AA3D Technology Sdn. Bhd. for their technical assistance and support.
| Filename | Description |
|---|---|
| R1-ME-6708-20230929144848.docx | Table of Correction |
Abas, M., Habib, T., Noor, S.,
Zimon, D., Wozniak, J., 2023. Application of Multi-criteria Decision-making
Methods in the Selection of Additive Manufacturing Materials for Solid Ankle
Foot Orthoses. Journal of Engineering Design, Volume 34(8), pp. 616–643
Abdullah, A.H., Rashid, H.,
Mahmud, J., Othman, M.F., Ibrahim, M.W.A.-J. 2012. Effects of Screw Materials
in Anterior Cruciate Ligament Reconstruction using Finite Element Analysis. Procedia
Engineering, Volume 41, pp. 1614–1619
Ahmad, M.A., Zulkifli, N.N.M.E.,
Shuib, S., Sulaiman, S.H., Abdullah, A.H., 2020. Finite Element Analysis of
Proximal Cement Fixation in Total Hip Arthroplasty. International Journal of
Technology, Volume 11(5), pp. 1046–1055
Ahmed, R.M., Al-Shammari, M.A.,
2023. EMG-Based Control of Active Ankle-Foot Prosthesis. Journal of
Engineering, Volume 29(9), pp. 31–44
Amitrano, F., Coccia, A., Pagano,
G., Biancardi, A., Tombolini, G., Daddio, G., 2023. Effects of Ankle-Foot
Orthosis on Balance of Foot Drop Patients. Studies in Health Technology and
Informatics, Volume 302, pp. 1029–1030
Cleveland Clinic, (n.d.).
Brachial Plexus Injuries. Available online at
https://my.clevelandclinic.org/health/diseases/22822-brachial-plexus-injury,
Accessed on January 25, 2023
Cutti, A.G., Morosato, F.,
Gentile, C., Gariboldi, F., Hamoui, G., Santi, M.G., Teti, G., Gruppioni, E.,
2023. A Workflow for Studying the Stump–Socket Interface in Persons with
Transtibial Amputation through 3D Thermographic Mapping. Sensors, Volume
23(11), p. 5035
Devin, K.M., Tang, J., Moser, D.,
Jiang, L., 2023. Assessing Socket Fit Effects on Pressure And Shear at
aTranstibial Residuum/Socket Interface. Applied Bionics and Biomechanics,
Volume 2023, p. 3257059
Faadhila, A., Rahman, S.F.,
Whulanza, Y., Supriadi, S., Tampubolon, J.Y., Wicaksana, S.I., Rahyussalim,
A.J., Kurniawati, T., Abdullah, A.H., 2022. Design of a Transforaminal Lumbar
Interbody Fusion (TLIF) Spine Cage. International Journal of Technology,
Volume 13(8), pp. 1663–1671
Farah, S., Anderson, D.G.,
Langer, R., 2016. Physical and Mechanical Properties of PLA, And Their
Functions in Widespread Applications — A Comprehensive Review. Advanced Drug
Delivery Reviews, Volume 107, pp. 367–392
Hamza, S., Heidari, M.,
Ahmadizadeh, M., Dashtizadeh, M., Chitt, M., 2023. Modification of Horizontal
Wind Turbine Blade: A Finite Element Analysis, International Journal of
Technology, Volume 14(1), pp. 5–14
Hamzah, S.R., Nor-Izmin, N.A.,
Tardan, G., Abdullah, A.H., 2019. Design and Analysis of Adjustable Headrest
for Total Body Involvement Cerebral Palsy, International Journal of Recent
Technology and Engineering, Volume 8(1), pp. 3208–3211
Johns Hopkins Medicine, (n.d.).
Brachial Plexus Injury. Available online at https://www.hopkinsmedicine.org/
health/conditions-and- diseases/ brachial-plexus-injuries, Accessed on January 25,
2023
Jonnala,
U.K., Sankineni, R., Kumar, Y.R., 2023. Design and
Development of Fused Deposition Modeling (FDM) 3D-Printed Orthotic Insole by
Using Gyroid Structure. Journal of the Mechanical Behavior of Biomedical
Materials, Volume 145, p. 106005
Levesque, L., Doumit, M. 2020.
Study of Human-Machine Physical Interface for Wearable Mobility Assist Devices.
Medical Engineering & Physics, Volume 80, pp. 33–43
Mazlan, M.A., Anas, M.A.,
Nor-Izmin, N.A., Abdullah, A.H. 2023. Effects of Infill Density, Wall Perimeter
and Layer Height in Fabricating 3D Printing Products. Materials, Volume
17, p. 695
Mazlan, M.A., Hashim, N.M.,
Zakaria N.A.C., Abdullah, A.H. 2021. 3D Printed Assistive Writing Device for
Phocomelia Patient. Malaysian Journal of Medicine and Health Sciences,
Volume 17(13), pp. 7–11
Moreland, D.W., 2009. Mechanical
Systems Safety. In: Safety Design for Space Systems, Musgrave, G.E.,
Larsen, A.M., Sgobba, T., (ed.), Elsevier Science
National Institute of
Neurological Disorders and Stroke, 2008. NINDS Brachial Plexus Injuries, 2008
Nigro, L., Arch, E.S., 2023.
Design and Mechanical Testing of a Novel Dual-Stiffness Ankle-Foot Orthosis. Journal
of Medical Devices, Volume 17(3), p. 034501
Nor-Izmin, N.A., Hazwani, F.,
Abdullah, A.H., Todo, M., 2020. Risk of Bone Fracture in Resurfacing Hip
Arthroplasty at Varus and Valgus Implant Placements. International Journal
of Technology, Volume 11(5), pp. 1025–1035
Oliver, M., 2019. Assistive
Technology in Polytrauma Rehabilitation. Physical Medicine and
Rehabilitation Clinics, Volume 30(1), pp. 217–259
Rashid, H., Ariffin, M.K.M., Noh,
M.H.M., Abdullah, A.H., Hamid, A.H.A., Jusoh, M.A.M., Othman, A., 2012. Design
Review of Scissors Lifts Structure for Commercial Aircraft Ground Support
Equipment Using Finite Element Analysis. Procedia Engineering, Volume
41, pp. 1696–1701
Sarma, T., Saxena, K.S., Majhi,
V., Pandey, D., Sahai, N., 2020. Development Of Active Ankle Foot Orthotic
Device. Materials Today: Proceedings, Volume 26(2), pp. 918–921
Scherb, D., Steck, P., Wechsler,
I., Wartzack, S., Miehling, J., 2023. The Determination of Assistance-as-Needed
Support by an Ankle–Foot Orthosis for Patients with Foot Drop. International
Journal of Environmental Research and Public Health, Volume 20(17), p. 6687
Sousa, R.,
Pereira, A., Massada, M., Trigueiros, M., Lemos, R., Silva, C., 2011. Shoulder
Arthrodesis in Adult Brachial Plexus Injury: What is The Optimal Position? Journal
of Hand Surgery, Volume 36(7), pp. 541–547
Volpi, M., Paradiso, A.,
Costantini, M., Swieszkowski, W., 2022. Hydrogel-based Fiber Biofabrication
Techniques for Skeletal Muscle Tissue Engineering. ACS Biomaterials Science
& Engineering, Volume 8(2), pp. 379–405
Wahid, A.M.A., Tardan, G.,
Pangesty, A.I., Rashid H., Abdullah, A.H., 2022. Development of Ankle-Foot
Orthosis with the Integration of IoT Controller. International Journal of
Emerging Technology and Advanced Engineering, Volume 12(5), pp. 49–55
